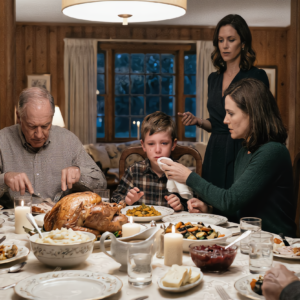She was still wearing her cleaning uniform when she carried her seven-year-old into the ER.
Her name patch was peeling. Her sandals were cheap. Her hair was falling out of its knot. And in her arms, her son was burning up and struggling to breathe.
She stepped to the desk and said, “My son needs help.”
The doctor looked at her uniform, her shoes, her tired face — and said,
“If you don’t have money, don’t push your way in here.”
Not one question about the fever.
Not one question about the breathing.
Not one question about the child.
Just judgment.
But the mother didn’t beg.
Not this time.
Three years earlier, she had begged in that same hospital while her daughter died waiting to be seen. Since then, she had spent years quietly gathering proof that poor families were being delayed while better-dressed ones moved faster.
So when the doctor dismissed her sick son, she pulled out an old flip phone and made one call:
“Tell Rachel Stein the mother from St. Vincent’s East has her final proof.
And my son still needs a doctor.”
That was the moment the room changed.
A nurse finally stepped in.
The child’s oxygen was already crashing.
Severe pneumonia. Early sepsis. Minutes from becoming another “tragic outcome.”
And suddenly the hospital that looked at her sandals before it looked at her son had a much bigger problem than one angry mother.
Because she wasn’t just a scared parent.
She was the woman who had spent three years inside that system, watching, documenting, and counting every time they asked poor families about payment before they asked what hurt.
They thought she was invisible.
They were wrong.
And by the time the night was over, she hadn’t just saved her son.
She had exposed the whole building.

The mother was still wearing her cleaning uniform when she carried her son into the emergency room.
The blue scrub top was damp at the collar.
Her name patch—MARISOL—was half-peeled at one corner from too many industrial wash cycles. Her hair was pulled into a knot that had started the evening tight and ended it loose. The plastic sandals on her feet were cheap white ones with the heels worn down crooked from years of standing on wet floors.
In her arms, her son burned.
Mateo’s face was flushed an impossible red. His head rolled against her shoulder with the boneless heaviness of a child too sick to hold himself up. His breaths came fast and shallow, each one with a small catching sound that made her stomach feel lined with nails.
The emergency department at St. Vincent’s East was bright in the cruel way hospitals often are after midnight. Too much fluorescent light. Too much polish on the floor. Too much chill in the air to ever let anyone forget they were in a place where suffering was processed by shift.
A television mounted high in the corner was talking about election polling with the sound off.
At the intake desk, a woman in navy scrubs was typing.
Behind her stood Dr. Alan Mercer, the attending physician on duty. Mid-fifties. Crisp beard. White coat. The kind of face people trusted without realizing how often they were trusting a performance.
Marisol stepped up to the counter and said, “My son needs help.”
The intake clerk looked up first.
Then the doctor.
And Marisol watched the exact moment his eyes dropped—not to Mateo’s face, not to the boy’s breathing, not to the hand limp against her shoulder—but to Marisol’s shirt, the cheap sandals, the cleaning chemicals dried white at the cuff of her sleeve.
He didn’t even try to hide the judgment.
“If you don’t have money,” he said, “don’t push your way in here.”
The sentence fell across the room like a tray dropped in church.
The clerk froze.
A teenager in a wrist brace stopped scrolling on his phone.
An old man in the corner turned his head.
A pregnant woman sitting with a blanket over her lap looked up so fast her hand went to her mouth.
Nobody said anything.
That was the worst part.
Not the cruelty.
The familiarity of it.
No one asked how long the boy had been sick.
No one asked whether he had a history of asthma, seizures, pneumonia, heart trouble, allergies.
No one asked if he was breathing evenly.
No one asked anything that would have sounded like medicine.
Marisol stood there with thirty-eight pounds of fevered child in her arms and did not beg.
Three years earlier, she would have begged.
Three years earlier, she had.
It had not saved anyone.
So she lowered Mateo carefully onto one of the plastic waiting-room chairs.
His body slumped sideways. His breath hitched.
A young nurse near the triage station looked over sharply.
Marisol reached into the chest pocket of her uniform and took out an old flip phone with scratches across the hinge.
She pressed one number from memory.
Waited.
When the call connected, she didn’t raise her voice.
She said, “Tell Rachel Stein the mother from St. Vincent’s East has her final proof.”
Then, after one beat:
“And my son still needs a doctor.”
Nurse Ava Bell had been watching before anyone realized she was.
She was twenty-nine, twelve months into emergency nursing, and still new enough to hate the things older staff had learned to call normal. She’d seen parents panic over splinters and nosebleeds and fevers that turned out to be nothing worse than a bad virus. She had also seen children crash with terrifying speed while adults argued over insurance at the desk.
The boy in the chair was not nothing.
She crossed the floor before Dr. Mercer could decide whether to stop her.
“What’s his name?” she asked.
Marisol looked up. Her eyes were dry, alert, and exhausted in a way Ava recognized from her own mother’s face years ago after double shifts and bills nobody could stretch anymore.
“Mateo.”
“How old?”
“Seven.”
“How long has he had the fever?”
“Since this morning. Worse in the afternoon. He started breathing fast an hour ago.”
Ava crouched and put two fingers lightly to the side of Mateo’s neck. Hot skin. Rapid pulse. She leaned close enough to hear the breathing. Too fast. Too shallow. His lips were dry. His shirt clung to his chest with sweat.
“Has he been vomiting?”
“Twice.”
“Can he wake up?”
Marisol touched the boy’s cheek.
“Mateo.”
His eyelids fluttered. He made a soft sound, not quite a word.
Ava looked up toward the desk. “We need a room.”
Mercer did not move.
“Get his information first.”
Ava stared at him.
“He’s breathing thirty-eight to forty times a minute.”
“We don’t know his baseline.”
“He’s seven.”
“He’s also not cyanotic, and we have two higher-acuity rooms tied up.”
The old man in the corner had begun watching openly now.
So had everyone else.
Because once a room senses something wrong, it cannot un-feel it.
Marisol stood very still.
Ava said, lower now, “He’s lethargic.”
Mercer’s mouth tightened.
“Vitals in triage.”
Marisol could have accepted that.
Triage was at least medicine-adjacent.
But the intake clerk, rattled by the call she had just overheard and clinging to the script that kept the room ordered, pushed a clipboard across the counter and said, “Insurance card and ID first, please.”
Ava actually laughed once, out of disbelief more than humor.
Marisol did not.
She slid the clipboard back without looking at it.
“My son is trying to breathe,” she said.
Mercer folded his arms.
“Everyone here is waiting.”
“No,” Marisol said quietly. “Everyone here is visible.”
The line hung in the fluorescent air.
Mercer heard it. So did Ava.
So did the pregnant woman in the blanket, who looked down at her own hands immediately, like she had been caught in a truth she had not earned the right to examine.
Ava stepped forward.
“Room five,” she said.
Mercer turned.
“That is not your call.”
Ava did not back up. “Then make it yours.”
Before he could answer, Mateo’s head rolled back against the chair.
His body gave one short, violent shiver.
Then another.
Ava swore under her breath.
“Now.”
Everything sped up at once after that.
The waiting room never forgives a child for proving an adult wrong in real time.
Mercer moved. Not quickly enough to erase the previous three minutes, but quickly enough to become a doctor again. A tech appeared with a wheelchair. Ava and Marisol lifted Mateo together. His skin was scorching. His breathing had gone ragged now, each inhale sharp enough to pull the skin between his ribs inward.
Room five.
Pulse oximeter.
Blood pressure.
Monitor leads.
Ava clipped the sensor onto his finger and felt her throat tighten.
Oxygen: 88.
“Nonrebreather,” she snapped.
Mercer was at the bedside now, stethoscope out, no trace left of the man who had been at the desk except the damage.
“Lungs sound terrible.”
Ava gave him a flat look she did not bother to hide.
Marisol stood on the other side of the bed, one hand on Mateo’s ankle under the blanket, as if keeping contact with one small part of him might keep the rest from slipping.
“Possible pneumonia,” Mercer said. “Possible sepsis. CBC, CMP, lactate, blood cultures, chest film, fluids, ceftriaxone, respiratory.”
He was ordering fast now.
He was also hearing his own voice in the room for what it was worth when spoken after delay.
Not enough.
Nothing in medicine becomes clean just because urgency eventually arrives.
Mateo coughed once under the oxygen mask, and the sound seemed too small for how sick he was.
Ava reached for the IV supplies.
“Mom, stay by his shoulder. Keep talking to him.”
Marisol nodded.
“Mateo. Baby, listen to me.”
Her voice changed when it turned toward her son.
That always happened.
The room saw the worker first. The system saw the clothes first. The doctor saw the sandals first.
But a mother’s voice always knows where to go.
“You’re okay,” she said, though he wasn’t. “You hear me? You breathe. You stay with me.”
When Ava slid the IV into the back of Mateo’s hand, the boy barely flinched.
That frightened her more than anything else so far.
At the door, a unit secretary stepped in and said quietly, “There’s someone here asking for the chief administrator. Says she’s with the Children’s Bridge Foundation.”
Mercer looked up.
Ava looked at Marisol.
Marisol did not look surprised.
“Good,” she said. “She’s on time.”
Three years earlier, Marisol Vega had believed that hospitals told the truth.
Maybe not kindly.
Maybe not quickly.
But truthfully.
That had been before her daughter Sofia.
Sofia was four and loved yellow things with the seriousness some children reserve for religion. Yellow rain boots. Yellow crayons. A yellow plastic cup she insisted made orange juice taste better. When she got sick, Marisol thought at first it was flu.
Fever.
Sleepiness.
A little vomiting.
Then her neck hurt. Then the fever climbed. Then Sofia stopped complaining and only whimpered, which turned out to be worse.
Marisol had brought her to St. Vincent’s East because it was the closest place that took walk-ins and because when you are a mother with one child burning in your arms and another asleep at home with a neighbor, distance becomes a theology.
That night she had still believed in pleading.
“Please,” she had said at the desk. “Please look at her.”
The clerk had asked for insurance.
The woman beside her had asked if Sofia had a pediatrician.
The nurse in triage had written fever x 1 day without looking up.
They had waited.
And waited.
A toddler with a private urgent care wristband had been taken back before them because his mother knew the language of complaint. A businessman with chest discomfort had been wheeled immediately through because his watch spoke the dialect of liability. A girl with a soccer concussion was roomed within minutes because her father said “I donate” into his phone while standing in line.
Sofia lay across three waiting-room chairs and stared at the TV without blinking much.
When she finally seized, it happened so fast Marisol thought at first she was choking.
Then too many people arrived at once.
Then not enough of the right things happened in time.
Meningococcal sepsis, someone said later.
Fulminant.
Aggressive.
Difficult to catch early.
One of the doctors used the phrase “even with prompt intervention,” which Marisol came to hate with a private and blistering precision.
Even with prompt intervention.
As if prompt had belonged to them that night.
As if prompt had not become a privilege distributed by appearance, language, paperwork, and the invisible wage line in a parent’s voice.
Sofia died twenty-six hours later in a pediatric ICU room with cartoon fish on the wall and tape marks on both hands where they had tried too late to save what the waiting room had already spent.
After the funeral, people said things meant to comfort.
God needed another angel.
She’s no longer suffering.
At least you still have Mateo.
At least.
Marisol nearly slapped the third person who said that.
Instead she stopped believing in at least.
And stopped believing that what had happened to Sofia was one terrible exception.
Because once grief stops screaming, it begins noticing.
In the months after the funeral, she kept returning to St. Vincent’s East for Mateo’s follow-up asthma visits. Each time she saw some version of the same rhythm.
Well-dressed parents moved faster.
Parents who spoke confident English moved faster.
Families who arrived with employer insurance cards already in hand moved faster.
The poor were told to sit. Fill this out. Wait. Calm down. Don’t crowd the desk. Someone will call you.
Her old faith in hospitals did not vanish all at once.
It soured.
And sour things become questions.
The first question she asked was too small for anybody else to hear:
How often does this happen?
The second question changed her life:
Who would care enough to count it?
The answer came six months later from a woman in a navy suit at a church legal aid clinic downtown.
Rachel Stein did not look like the kind of person who received grieving mothers every day.
She looked expensive in a clean, deliberate way. But her eyes were the eyes of someone who had heard too many polished explanations and stopped mistaking them for truth years ago.
She headed the Children’s Bridge Foundation, a private nonprofit that funded pediatric access programs, family advocates, and emergency grants across three counties. On paper the foundation was charitable.
In reality, it was also nosy in the most useful sense.
They had been hearing things about St. Vincent’s East for years.
Stories.
Patterns.
Nothing clean enough for court and nothing dramatic enough for public outrage.
Not yet.
Rachel had listened to Marisol for forty-three minutes without interrupting once.
Then she’d asked one question.
“Do you want compensation,” she said, “or do you want to know whether Sofia was alone?”
Marisol had stared at her.
Rachel leaned forward.
“Because those are different roads. I can help you down one. Maybe not both.”
Marisol took home that question like a stone too heavy for one hand.
Three weeks later, she called Rachel back and said, “I want to know if they do this to other children.”
That was how it started.
Not with revenge.
With counting.
At first Marisol did not work inside the hospital.
She cleaned office buildings downtown at night and a dental clinic on Saturdays. She was barely keeping rent steady and Mateo clothed and her mother’s medication box filled. Working as a housekeeper on the St. Vincent’s East campus came a year later, after the private contracting company lost a staff member in the surgical tower and posted overnight openings.
Marisol took one look at the listing and understood two things at once.
She needed the money.
And invisibility has access.
The thing institutions forget about cleaners is that the whole building speaks around them.
Doctors do not lower their voices near the woman emptying the sharps overflow bin. Administrators don’t stop mid-sentence because a floor buffer is humming at the end of the hall. Billing staff don’t think the woman wiping coffee rings from a conference table can map power by which names make them laugh and which make them whisper.
For three years Marisol moved through St. Vincent’s East with a mop handle in one hand and memory sharper than most clipboards.
She learned shift patterns first.
Which nights the pediatric ER backed up.
Which doctors rounded late.
Which registration clerks asked for payment information before symptoms even when policy said not to.
Which charge nurses corrected that and which ones pretended not to notice.
She never stole charts.
Never photographed anything that would put an individual child’s private medical record in danger.
Rachel had been clear about that from the beginning.
“We expose systems,” she said. “We do not become one more thing that violates families.”
So Marisol counted what systems reveal publicly.
Arrival times.
Time to triage.
Time to first provider.
Insurance questions asked before vitals.
The phrases people used when they assumed no one who mattered was listening.
Self-pay family.
Probably just another fever.
These people always wait until it’s bad.
Charity case.
Medicaid. They can sit.
Every Friday she called a number Rachel gave her and left a voicemail with coded details that later became spreadsheets.
Blue shoes meant pediatric delay.
Window three meant Mercer.
Yellow bracelet meant uninsured.
Sixteen minutes.
Thirty-two minutes.
Forty-nine.
Mother crying.
Child vomiting.
Payment asked first.
Sometimes Rachel met her in the back pews of Saint Agnes after mass and took handwritten notes folded inside the church bulletin.
Sometimes they met in the parking lot of a grocery store, where Rachel sat in her car in pearls and orthopedic shoes like somebody’s aunt and accepted details that made her jaw go hard.
Three years built a pattern.
Not perfect.
Patterns never are.
But enough.
Enough that Children’s Bridge began a quiet review of St. Vincent’s East’s pediatric emergency grant compliance. Enough that Rachel started asking harder questions of the hospital’s board when they came requesting a new foundation partnership for a much-photographed children’s wing renovation. Enough that lawyers began talking about statistical disparity in intake timing tied to insurance and race proxies.
They were close.
What they lacked was a case no one could explain away as anecdote.
A live one.
A documented one.
A final proof.
Marisol never wanted it to be her son.
But systems don’t care what proof costs the people gathering it.
In room five, Mateo’s fever came back at 105.1 rectally.
Ava hung the second bag of fluids while respiratory adjusted the mask and a portable chest x-ray plate slid beneath the boy’s back.
Mercer listened to the lungs again.
“Right lower lobe sounds awful.”
Ava said nothing.
The labs started coming.
White count high. Lactate elevated. Blood pressure softening. Oxygen better with support but not enough to relax anyone honest.
Mercer cursed under his breath.
Severe pneumonia, likely septic progression.
Treatable.
Dangerous.
And dangerously close to having been one more delayed child in a room full of adults convinced delay was a neutral act.
The door opened.
Rachel Stein came in with the sort of calm that always makes guilty people start explaining before anyone has asked a question.
She was in a charcoal coat over a black dress, hair still pinned from whatever meeting Marisol’s call had interrupted. Beside her stood a man with a slim briefcase and state-bar confidence—foundation counsel, apparently—and behind them the hospital’s chief administrator, Donna Kelley, pale and already out of breath.
“Marisol.”
Rachel crossed the room first, not to the doctor or the administrator, but straight to the bed.
She looked at Mateo for two seconds and then at Ava.
“Is he stable?”
“Not yet.”
Rachel nodded once, absorbing that the timeline in her head had just changed from legal to maternal.
She touched Marisol’s arm.
“You did the right thing.”
Marisol looked at her.
“No,” she said. “I did the only thing left.”
Donna Kelley took a step forward.
“I understand there’s been some kind of misunderstanding—”
Rachel turned.
There are people who know how to lower a room’s temperature without raising their voice. Rachel Stein had made a career of it.
“A child with sepsis symptoms sat at your intake desk while one of your physicians assessed his mother’s footwear before assessing his breathing,” she said. “Choose a better opening.”
Donna stopped.
Mercer drew himself up. “I am actively treating him now.”
Rachel faced him fully.
“Doctor, if a fire crew stands around discussing whether the family can afford water before they turn on the hose, the fact that they eventually spray does not become the headline.”
Ava almost looked impressed despite herself.
Mercer’s ears reddened.
He opened his mouth. Closed it.
Good, Rachel thought. Shame might yet save him from saying something even worse.
The lawyer beside her, David Rosen, set his briefcase on the counter.
“For the record,” he said, “we are preserving all intake footage from tonight, all audio from desk microphones, all EHR access logs, and all staffing assignments.”
Donna Kelley turned toward him. “You can’t simply—”
“We can request, compel, subpoena, and publicize,” David said pleasantly. “Tonight you get to pick which route sounds least exhausting.”
Marisol never took her hand from Mateo’s ankle.
She had long ago learned that when institutions start speaking legal, children can disappear again inside the grammar.
So she said the one thing that made the room face the bed.
“My son first.”
Ava nodded immediately.
“Yes.”
Mercer looked at the monitor. Oxygen inching up. Heart rate still racing. Fever still brutal.
He stripped the white coat off and hung it on the back of the chair.
That would not save him.
But it did make him look less like authority and more like one tired man standing in the consequences of himself.
“I need a blood gas and repeat vitals in fifteen,” he said.
Ava moved.
Rachel stayed beside Marisol.
“What do you need?”
Marisol took a slow breath.
“For him to breathe through the night.”
Rachel’s face softened, just once.
“Then that’s what we do first.”
Mateo got his first full sentence back at 3:17 a.m.
It came after three hours of fluids, antibiotics, oxygen, a pediatric ICU consult, one near-intubation scare, and two terrifying moments when his blood pressure dipped low enough that Ava’s heartbeat seemed to relocate into her throat.
His eyelids fluttered.
He looked at Marisol through the oxygen mask and whispered, “Mama?”
The room changed.
It always does when the child returns.
Not cured.
Not safe.
Just back enough to ask for the person who carried him there.
Marisol bent so fast her back protested.
“I’m here.”
He swallowed painfully.
“Cold.”
Ava found a warm blanket and tucked it around him.
Mateo’s hand searched weakly under the sheet until it found Marisol’s wrist and stayed there.
Mercer left the room for the first time in nearly an hour.
Not because he was done.
Because he needed the hallway.
Ava followed him out after finishing the chart entry.
He stood near the supply cart with both hands braced on his hips, staring at the floor.
“You knew he was sick,” Ava said.
Mercer did not look up.
“Yes.”
“Not fast enough.”
No answer.
Ava had not known him long, but she knew enough. Mercer liked being the adult in the room. The practical one. The one who didn’t sentimentalize medicine. He would have told you that emotion killed efficiency and that he’d spent twenty years learning not to be manipulated by panic.
She also knew that men like him often used the word manipulated when they meant made uncomfortable by poor people.
He said, finally, “I made a judgment.”
Ava leaned against the wall.
“You made a category.”
He looked at her then.
Maybe to correct her.
Maybe because he knew she was right.
“He is receiving excellent care now,” he said.
Ava’s face went flat.
“That’s the thing about late mercy,” she said. “It always wants credit for arriving.”
He flinched.
Good, she thought. Let it sting where it belongs.
Down the hall, two administrators walked quickly past toward the conference suite, already gathering themselves around the shape of future damage.
Ava watched them go.
“This isn’t just tonight, is it?”
Mercer said nothing.
“That mother,” Ava went on, lower now, “didn’t walk in scared the way people usually are when they think the hospital might save them. She walked in ready.”
He looked back toward room five.
“Yes.”
“And whatever comes next,” Ava said, “we earned it.”
At 4:05 a.m., with Mateo more stable and asleep under warm blankets, Rachel asked Marisol if she could step into the family consult room for ten minutes.
Marisol hesitated.
Ava said, “I’ll sit with him.”
That was enough.
The consult room had the usual hospital attempt at softness. Beige walls. Two armchairs nobody would willingly keep at home. A framed watercolor of boats no one looked at. A box of tissues placed with such aggressive optimism it bordered on insult.
Donna Kelley was already there with the hospital’s legal counsel and a board liaison named Stephen Harlan who had probably never expected to meet the janitorial subcontractor whose testimony might blow up their pediatric expansion campaign.
Rachel sat down first.
Marisol remained standing until Rachel said, gently, “Sit. You’ve been on your feet since before sunset.”
Marisol sat.
David Rosen opened a folder.
“Here’s where we are,” he said. “Three years of internal observation from Ms. Vega. Pattern data from public grant reporting. Tonight’s recorded denial and delayed triage. Staff witness. Potential injury outcome if there had been further delay.”
Stephen Harlan rubbed his forehead. “This can’t be happening.”
Rachel looked at him.
“It has been happening,” she said. “That’s the point.”
Donna Kelley straightened in the chair.
“St. Vincent’s East serves thousands of families every month. We are under immense pressure. Individual incidents—”
Rachel actually smiled.
It was not a kind smile.
“Administrator Kelley, your hospital applied for twenty-two million dollars in pediatric access support six months ago using language about equity, early intervention, and family-first emergency care. I helped write the funding standards you signed.”
Donna opened her mouth.
Rachel lifted a hand.
“Do not insult me with the phrase individual incidents until you have reviewed the dataset your housekeeping staff has been building while your physicians spoke around her like class was a diagnosis.”
The room went still.
Stephen Harlan turned toward Marisol as if seeing her for the first time.
That was the humiliation of it.
She had worked in their building for three years.
He had probably walked past her cleaning a spill outside executive conference room B more than once.
Invisible labor is most offensive to powerful people when it stops being invisible on command.
Marisol looked back at him without helping.
Donna tried again.
“We will investigate fully.”
“No,” Marisol said.
It was the first time she had spoken since sitting down.
Everyone turned.
She folded her hands together once on the table because they were starting to shake, and she did not want the shake mistaken for weakness.
“Three years ago,” she said, “I begged in your waiting room while my daughter burned up in a chair. Tonight I did not come here for an investigation. I came here because my son was sick.”
Her voice did not rise.
That made it worse for them.
“You made it a case again,” she said. “Not me.”
Rachel said nothing.
David said nothing.
Good lawyers know when the truth is already winning.
Marisol continued.
“I have scrubbed vomit off the pediatric hallway tile at two in the morning while children with better shoes got roomed faster than children with fever. I have emptied trash in administration after meetings where the words underserved families were printed in color on glossy slides. I have watched your staff ask for payment before they ask what hurts.”
Donna Kelley looked ill now.
Stephen Harlan could not seem to stop staring at Marisol’s hands, which were red and cracked from bleach and hot water and winter air and too much life done without gloves that fit.
Marisol leaned forward the slightest bit.
“You want to know what final proof means?”
No one answered.
“It means my son came in dangerous and your doctor saw my sandals before he saw his breathing.”
The sentence landed and stayed.
Rachel finally spoke.
“Children’s Bridge is suspending all pending grant consideration until this matter is independently reviewed. We are also notifying the state pediatric access board, county health oversight, and the attorney general’s healthcare equity unit.”
Donna inhaled sharply. “That will destroy—”
Rachel looked at her.
“What exactly?”
No one in the room volunteered the answer, though several knew it.
The campaign. The expansion. The philanthropic dinners. The glossy newsletter language. The illusion.
Good, Rachel thought. Let them say it plain in their own heads if they want relief.
Marisol sat back.
The rage she’d carried for three years had changed shape too many times now to be dramatic. It was not flame anymore. It was iron.
“I don’t want money first,” she said.
That made them all look up again.
“Not first?”
“No.”
David glanced sideways at Rachel, who gave the smallest nod. Let her lead.
Marisol looked from face to face.
“I want no child asked about payment before being medically assessed.”
She held up one finger.
“I want a pediatric advocate at intake on nights and weekends.”
A second finger.
“I want wait times audited by insurance status, language, and outcome.”
Third.
“I want intake footage reviewed any time a child deteriorates in the waiting room.”
Fourth.
“I want your staff retrained by people who know the difference between policy and prejudice.”
Fifth.
“And I want every mother who comes in dressed like she just left work to be treated like a mother, not a delay.”
No one wrote that down because no one there had paper in hand. But all of them remembered it.
Rachel looked at Marisol with something beyond respect now.
Not surprise.
Recognition.
There it was again, the thing she had seen three years ago across a folding table at legal aid. Marisol was not a woman who had stumbled into justice. She was a woman who had carried it in pieces until someone with money and credentials could no longer pretend not to see the shape.
Stephen Harlan cleared his throat.
“We can discuss implementation.”
Marisol looked at him.
“No,” she said. “You can agree, or you can explain to the cameras why a cleaning woman had to teach your children’s hospital what a sick child looks like.”
That ended the discussion portion of the meeting.
News did not break all at once the next morning.
It leaked in layers.
The video from intake.
The delayed rooming.
The Foundation statement.
The revelation that the mother at the center of the case had been a contracted worker on the St. Vincent’s East campus for years and had quietly cooperated in a broader equity review.
By noon, the story had outrun the hospital’s first PR response.
By two, a local paper published the line that would follow the hospital for months:
THEY LOOKED AT HER SHOES BEFORE THEY LOOKED AT HER SON.
Rachel hated viral lines on principle.
She also knew when one was deserved.
Mateo was transferred to pediatric step-down by afternoon. His oxygen needs were improving. The antibiotics were working. He was still frighteningly tired, still running hot, but the color around his mouth had eased and the terrible suctioning effort of each breath had begun to soften.
Marisol did not leave his bedside.
Ava brought her coffee she didn’t ask for and crackers she didn’t want but ate anyway. The body is shameless about what it demands after terror; it will ask for salt while your heart is still shaking.
Mercer came in near six p.m. with the latest labs.
He had slept neither well nor enough.
He gave the update first. Stable. Better than last night. Cultures pending. Repeat chest film consistent with severe bacterial pneumonia, likely early sepsis successfully interrupted.
Marisol nodded once.
Interrupted.
That was another hospital word she would never hear cleanly again.
When he finished, Mercer did not leave.
He stood with the chart in his hand longer than necessary.
Finally he said, “I owe you an apology.”
Marisol looked at Mateo, not at him.
Mercer continued anyway.
“What I said at the desk was wrong.”
Silence.
He swallowed.
“And what I assumed before I examined him was worse.”
Ava, by the sink, stopped pretending to organize syringes.
Marisol turned then.
“You think the problem was the sentence.”
Mercer’s face changed.
Not because she had been cruel.
Because she had reached the real wound faster than he wanted.
“The sentence matters,” he said.
“No,” Marisol said. “The sentence is just the first time people like me are allowed to hear what you were already thinking.”
Ava looked down.
Mercer had no defense that would not sound like cowardice dressed in credentials.
So for once he did something better than defending himself.
He stayed silent.
Marisol’s voice remained quiet.
“Three years ago, I cried at your desk. Last night I didn’t. Do you know why?”
Mercer did not answer.
“Because grief taught me something your training didn’t.” She looked at him directly now. “Delay is never neutral to the people being delayed.”
He closed the chart.
“I know that.”
“No,” she said. “You know it as risk. I know it as a child.”
The words hit him hard enough that Ava saw him physically shift.
Good, she thought again. Let the right people carry the weight.
Mercer nodded once.
“You’re right.”
That was not enough.
But it was not nothing either.
And on some days in medicine, not nothing is the only honest place to begin.
When the state review opened, it found what Rachel had expected and what St. Vincent’s East had spent years teaching itself not to see clearly.
Poor families were not denied care in writing.
Hospitals rarely write their sins plainly enough for subpoenas to enjoy.
What the review found instead was pattern.
Children listed as self-pay or uninsured waited longer for triage in high-volume periods despite equivalent symptom clusters.
Spanish-speaking families were more likely to have payment or paperwork questions documented before first-provider contact.
Children later admitted to higher acuity units had, in too many cases, been initially classified low urgency when they arrived with parents coded in internal intake comments as “distressed,” “demanding,” or “limited resources.”
The hospital called these anomalies.
Rachel called them what they were.
A system teaching itself whom to hesitate around.
Marisol had no patience left for euphemism.
“They knew how to move fast,” she told one interviewer weeks later. “They just didn’t move that way for everyone.”
She did not do many interviews.
That was deliberate.
She understood something the hospital did not: stories become easier to digest the more often the same face is made to explain them.
Rachel handled most of the press.
Ava gave a statement through counsel when asked about the intake delay.
Mercer, to almost everyone’s surprise, chose not to hide behind legal language. He admitted misjudgment. He accepted suspension pending review. He cooperated in the audit, which did not redeem him but did make him more useful than many men in his position would have been.
Donna Kelley resigned two months later “to pursue other opportunities,” the cleanest lie in healthcare administration.
Stephen Harlan went on television looking thirty years older and announced a set of reforms Marisol had written more than the board ever would have admitted.
Symptom-first pediatric intake.
Financial screening prohibited before medical assessment in all emergency presentations involving minors.
Onsite family advocates during peak hours.
Independent bias review panel.
Quarterly public reporting on pediatric wait times by payer category and language access measures.
A scholarship fund in Sofia Vega’s name for community health workers.
That last one Marisol nearly refused.
Not because she didn’t love Sofia.
Because institutions often try to turn dead children into decorative lessons.
Rachel talked her through it over coffee in a diner booth at six in the morning after another hospital meeting that had gone long enough to become absurd.
“It doesn’t erase anything,” Rachel said.
“I know.”
“It doesn’t buy your silence.”
“I know.”
“It puts her name where they have to pass it.”
That mattered.
Marisol looked out the diner window for a long time.
Then nodded once.
“All right,” she said. “But no gala.”
Rachel laughed into her coffee.
“No gala.”
Mateo came home after six days.
He was thinner, softer, and temporarily obsessed with orange gelatin because it had been the only hospital food he trusted. He coughed for two more weeks and slept with the boneless abandon of children who have narrowly missed large things without knowing their full shape.
One night, maybe a month later, he asked from the couch, “Mama, did I almost die?”
Children do that.
They lob the true question into the room while you’re folding laundry.
Marisol put down the towel in her hand.
“You got very sick.”
“Did I almost die?”
She sat beside him.
The TV reflected faint blue on the dark apartment window. The kitchen smelled like rice and garlic and clean detergent.
“For a little while,” she said. “Yes.”
Mateo absorbed that with the unnerving seriousness of seven-year-olds.
“Did you get scared?”
She smiled without humor.
“Yes.”
He nodded.
Then, after a second: “But you were there.”
That broke something open in her more thoroughly than the ICU ever had.
Not because it was dramatic.
Because it was simple.
Children believe proximity is power.
Sometimes they are right.
She kissed his hair.
“Yes,” she said. “I was there.”
Later that night, after he was asleep, she stood in the narrow kitchen and cried so quietly that even she could barely hear it.
Not for the first time.
For the first time without helplessness in it.
There is a kind of grief that only appears when danger has finally passed and the body is no longer busy.
That night it arrived carrying both children.
Sofia, who had not been carried out in time.
Mateo, who had.
The difference between them was not love.
It was minutes.
And systems built from those minutes.
Six months after the night in the ER, Marisol returned to St. Vincent’s East by choice.
Not as a cleaner.
She never cleaned their floors again.
Children’s Bridge hired her as a family access liaison for three hospitals and one urgent care network. The title was too long and too clean, but the work suited her better than any polished phrase.
She met parents at intake.
Explained forms in English and Spanish.
Tracked symptoms-first compliance.
Taught staff what poor families already knew: that confusion looks rude when you’re exhausted, and fear looks angry when no one is answering you.
The first week she worked there officially, a man in landscaping boots rushed in with his daughter in his arms. The girl’s face was gray with asthma struggle. The father could barely get out more than “she can’t—she can’t—”
The intake clerk—a new one—looked up and said immediately, “Tell me what’s happening with her breathing.”
No insurance question.
No clipboard pushed forward first.
No appraisal of boots or shirt or accent.
Symptom first.
The words hit Marisol in the chest so hard she had to steady herself on the counter behind her.
The father never knew why the woman in the navy family-advocate badge looked suddenly unable to speak for a second.
That was all right.
Victories do not become less real because they are private.
Later that same day, she passed the new sign mounted above intake.
FOR ALL PEDIATRIC EMERGENCIES: MEDICAL ASSESSMENT COMES FIRST.
It was just acrylic and bolts.
Still, she stood there longer than necessary.
Ava found her.
“You okay?”
Marisol looked at the sign.
“No,” she said honestly.
Ava waited.
Then Marisol added, “Better than before.”
That was honest too.
Ava leaned against the wall beside her.
“I still hear that night sometimes,” she said. “The waiting room. What he said.”
Marisol nodded.
“I hear the silence after.”
Ava looked at her.
“That’s the part that gets me.”
“Me too.”
Because cruelty is rarely alone.
It usually arrives with witnesses who have forgotten how to interrupt it.
The hospital never became noble.
That would have made a tidy ending and a dishonest one.
Hospitals are full of tired people and rushed systems and moral shortcuts wearing practical shoes. Reform did not make St. Vincent’s East saintly. It made it more aware of where it had been ugly and slightly less able to lie about that ugliness.
Sometimes that is what progress looks like in institutions.
Not halos.
Friction.
Mercer returned after suspension under supervision and with restrictions. Some people thought he should have been fired. Some thought he had been made the scapegoat for a culture older than him. Both things held pieces of truth, which meant neither satisfied everyone.
He saw Marisol often after that.
They were polite.
Nothing more.
Once, after a parent advocate meeting, he stopped in the hallway and said, “The new triage times are holding.”
Marisol said, “Good.”
He nodded.
Then, after a long pause, “I still think about your son in that chair.”
She looked at him.
“Good,” she said again.
He accepted that as the whole conversation he was owed.
That was progress too.
Rachel Stein remained what she had always been: dangerous in expensive shoes.
She secured the public reporting requirements into the hospital’s final foundation agreement so no future administrator could quietly edit them out in a quarter no one was watching. She hired two more parent liaisons. She also threatened three other hospitals with audits, because once you shine light on one waiting room, the others start sweating.
She and Marisol developed a rhythm that looked almost like friendship if you did not know how much work built it.
Diner coffee after hearings.
Text messages at odd hours.
Window three asking for billing first again—documenting.
Saw new advocate stay late for Spanish-speaking family. Good.
Mateo fever today, but normal fever. Not scary fever.
Rachel once replied to that last one with: There should not have to be categories of fever for a mother.
Marisol stared at the message for a long time before putting the phone down.
Because there are.
There always will be.
Ordinary fever.
Then memory fever.
Then the fever that teaches you what every room around you is made of.
One year after the night at intake, St. Vincent’s East held no gala.
Marisol had made sure of that.
What they held instead was a public community forum in the pediatric waiting area after hours, plastic chairs set in rows, coffee in cardboard boxes, translators present, no valet parking, no donor wall banner behind the speakers.
The Sofia Vega Family Access Desk had been open for four months by then.
Its name sat on a brass plaque beside intake, small enough to miss if you rushed and large enough never to disappear entirely.
Marisol stood near the back while Rachel spoke briefly about access and accountability and what it meant when a hospital decided to listen before being forced.
Ava spoke about the first medical minute.
A father whose infant had been rapidly identified with RSV because an advocate escalated her triage spoke in Spanish with his daughter on his lap. A grandmother talked about not being asked for payment before her grandson’s broken wrist got splinted.
No one called it redemption.
Good.
That word flatters institutions too easily.
At the end, the floor opened for questions.
A woman in a hotel housekeeping uniform stood up in the third row. Her sneakers were wet from rain. Her little girl leaned against her shoulder asleep.
The woman said, voice shaking, “My son died in another hospital five years ago because they made us wait. I just want to ask—how do I know this place is different now?”
The room went still.
Some questions deserve stillness.
Marisol crossed to the aisle before anyone else moved.
She did not take the microphone.
She stood close enough for the woman to see her face without amplification and said, “You don’t know from a promise.”
The woman looked at her, frightened and tired.
Marisol went on.
“You know from what happens when you walk through the door with a child who needs help.” She glanced toward the intake desk. “You know from who gets asked about symptoms first. You know from who stands beside you while the room decides what kind of mother you are.”
She let that sit.
Then she said, very quietly, “And if they forget again, they won’t forget alone.”
The woman started crying.
Not loudly.
Just the tired, ashamed crying of someone who has spent years learning not to need too much in public.
Marisol took her hand.
The child on her shoulder never woke up.
Behind them, the sign above intake shone under the fluorescent light.
Medical assessment comes first.
It should never have needed to be revolutionary.
And yet there it was.
Later that night, after the chairs were folded and the last coffee box thrown away and the building had resumed its hum of ordinary maintenance, Marisol walked the length of the hallway outside pediatric emergency alone.
She knew these floors better than most administrators knew their own promises.
She had mopped blood from tile here.
Scrubbed marker off walls.
Emptied bins full of paper gowns and IV wrappers and half-eaten crackers and the leftovers of people’s worst nights.
For a long time this hallway had taught her the shape of power from below.
Now it taught her something else.
Not hope exactly.
Hope is too clean a word for what poor people practice.
This was closer to vigilance with company.
At the intake desk, the night clerk was resetting forms.
A mother came in carrying a boy in soccer cleats who was sobbing over a wrist bent in the wrong direction.
The clerk stood up immediately.
“What happened to his arm?”
Symptom first.
The mother answered through tears.
The boy got roomed within minutes.
No one asked for a card.
No one looked at shoes.
No one evaluated the cut of the mother’s sweatshirt before evaluating the child.
Marisol stood very still beside the hallway wall.
That was it.
That was the thing.
Not headlines.
Not Rachel’s lawsuits.
Not Mercer’s shame.
Not the board meetings.
Not even the plaque.
This.
The ordinary right thing happening fast enough that no one in the room had to earn it with a perfect accent, a steady voice, or a better pair of shoes.
Three years earlier, she had walked these same halls with grief like acid in her chest and a mop bucket beside her, listening to the building talk around her as if women like her only existed to erase messes other people made.
Now another mother had walked in scared and gotten a question about pain before a question about money.
That did not bring Sofia back.
Nothing ever would.
Justice is terrible at resurrection.
But it can, sometimes, stop a pattern from claiming the next child quite so easily.
Marisol touched the edge of her ID badge—the new one, with FAMILY ACCESS LIAISON printed under her name—and then let her hand drop.
Ava stepped out of room three and saw her standing there.
“You heading home?”
“In a minute.”
Ava looked toward the desk, where the wrist-injury mother was being escorted back.
Then back at Marisol.
“You know,” she said, “for what it’s worth, that happened because of you.”
Marisol watched the doors close behind the family.
“No,” she said. “It happened because they had to learn how expensive delay really is.”
Ava leaned against the frame.
“That sounds like a yes wearing work boots.”
For the first time that night, Marisol smiled.
Small.
Real.
Then she looked once more at the desk, the sign, the movement of staff who had learned at least one new reflex in the dark.
And in that hospital light, in the ordinary hour after a hard day, with the smell of disinfectant and coffee and rain-damp coats still hanging in the air, she finally let herself name the thing she had carried in silence since the night Mateo almost became her second dead child.
She had not walked into the ER that night to make a scene.
She had walked in carrying a burning boy and the last piece of proof.
The miracle was not that they finally saw her.
The miracle was that, afterward, a few more children were seen in time.
News
At the Veterans Day Ceremony, a Police Officer Shoved an Old Black Man Out of the Front Row and Told Him, “Not Your Place.” The Crowd Went Silent, the Band Kept Playing, and the Old Man Bent Down to Pick Up His Cap Like He Was Used to Public Shame. But They Had No Idea That the Man on the Pavement Was the One This Entire Ceremony Was Really About.
I hit the pavement before I even understood what had happened. My cap slid across the concrete while the band kept playing like dignity was just another thing that could be stepped over in public. And with half the town…
At a Veterans Cemetery, a Police Officer Shoved an Old Black Man Into the Mud for “Not Belonging” There. As Witnesses Stared and Cameras Rose, He Clutched His Broken Flowers and Said Only, “I Came to Keep a Promise.” But They Had No Idea That the Grave He Was Walking Toward Held a Truth This Town Had Buried for Decades.
He put his hand on my shoulder before I could lay the flowers down.Then he looked at my coat, my skin, my cane, and decided I did not belong in an American veterans cemetery.What broke me was not the mud….
At the ER, a Homeless Man Staggered In Begging for a Doctor, and the Staff Treated Him Like He Was Looking for a Bed, Not Help. After a Doctor Told Him, “This Is a Hospital, Not a Shelter,” the Whole Waiting Room Went Quiet and Looked Away. But They Had No Idea That One Phone Call Was About to Change Everything They Thought They Knew About Him.
They looked at my coat before they looked at my chest.By the time I said I was having chest pain, the room had already decided I was a problem instead of a patient.And in a hospital in America built to…
At Thanksgiving, My Sister-in-Law Snatched the Plate Out of My Son’s Hands and Called Him a Freeloader in Front of the Whole Family. Everyone Else Kept Eating Like Nothing Happened. But They Had No Idea That I Was About to Make One Quiet Decision That Would Change Everything for Them.
They took my nine-year-old son’s dinner before he even sat down.My sister-in-law called him a freeloader in front of the whole Thanksgiving table.And while the gravy kept moving like nothing had happened, I quietly canceled the deposit on the house…
At My Brother’s Funeral, They Treated Me Like Trash Because My Clothes Looked Poorer Than Their Grief. After They Forced Me Out and Let a Cop Call Me a “Suspicious Black Male,” No One Defended Me. But They Had No Idea That I Was the Brother Isaiah Had Been Searching For, and the K9 They Brought to Control Me Was About to Reveal the Truth.
They brought a police dog to my brother’s funeral before anyone bothered to ask who I was.An officer looked me in the face, outside a small funeral home in Alabama, and called me a suspicious Black man.And for one brutal…
After My Dog Went Missing for 3 Days, He Showed Up Wearing a Handwritten Bill for Broth, Eggs, Chicken, and One Stolen Meatloaf Sandwich. I Thought I Was About to Settle a Ridiculous Debt and Bring Home a Shameless Freeloader. The Whole Neighborhood Treated Him Like a Sweet Little Con Artist. But They Had No Idea That My Dog Had Been Secretly Building the Family None of Us Knew We Needed.
My dog disappeared for three days and came home wearing a bill tied to his collar.Not a tag. Not a shelter note. An actual handwritten list of food charges from somewhere in my neighborhood.And I swear, standing there on my…
End of content
No more pages to load